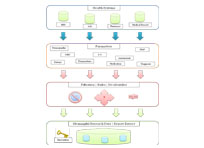
- Reserch Projects
- iCare/DocuCare
- Y-12 PDRD
- OKWA
- Mobile Learning
- Ongoing Efforts
- US-HAP
- HRSA
- SmartCare
- UTMC
- PLWHA
Feasibility of Electronic Data Capture from the Electronic Medical Records for Research Purposes and Validation of SIRS Scores
Principal Investigator: Dr. Reba Umberger, College of Nursing
Co-Investigator: Chayawat “Yo” Indranoi, MIE, University Health Services
Project Synopsis:
The goal of this three-phase pilot project was to evaluate and validate electronic data capture methods from the electronic medical records in planning for a large observational study.
Data collection in a large clinical trial can present multiple challenges regarding consistency in data quality, personnel time, and costs. The electronic medical record (EMR) provides the opportunity to gather large amounts of data for research purposes and reduce data entry errors that could occur with manual collection and entry of data. The use of the EMR for research has become more frequent over the past decade. A review of 126 studies suggests best approaches and challenges as we engage the EMR for research purposes and move away from merely using administrative data databases (Dean et al., 2009). Research uses of the EMR range from identification of research subjects in screening for conventional trials to actually being the focus of research by large managed care organizations. A lack of standardization across platforms limits comparability across EMR systems; and, potential system changes within one EMR may provide challenges. Typically, the EMR is used as the gold standard for comparison in validation studies; however, we recognize that this is limited by the data entry capabilities available to providers and the data that are entered.
For this study, we tested the feasibility to capture specific data that may be needed for a larger study. In addition, we validated the ability to abstract Systemic Inflammatory Response Syndrome (SIRS) score component variables. SIRS is a physiologic manifestation in response to an infectious or non-infectious insult. The Cerner System, used by UTMC, provided a tool that allowed nurses to readily select for the presence of SIRS component variables, and then calculate and record the score into the EMR. Monitoring SIRS can be used as an early warning sign of Sepsis. The MCC unit nurses implemented this practice and calculated SIRS scores every 12 hours beginning in September 2012 and continued until February 2013 when they further implemented a Cerner tool known as the St. John Sepsis Agent ( https://store.cerner.com/items/1527 ). This tool allows participating hospitals to customize the “agent” which searches through the EMR based on an algorithm for severe sepsis (SIRS plus organ failure). The presence of specific criteria triggers a required task for the nurse to notify the MD and team leader. Depending on a patient’s admission diagnoses and prior triggers/alerts, the “agent” is suppressed for a customizable time period (such as 48 hours). MD and team leader notifications are recorded in the EMR – although the scores are not readily viewable from within Cerner. SIRS scores are relevant to future planned research; therefore, we validated the ability to capture SIRS component variables. Through this project, we were able to report the implementation of the sepsis “agent” triggers alerts. This scope of this project was limited and did not extend to the cause and treatment of sepsis.
Publications/Presentations